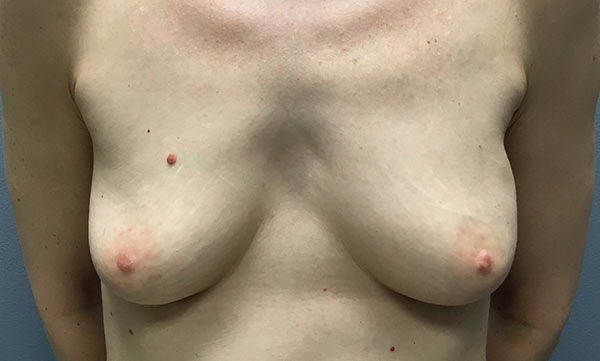
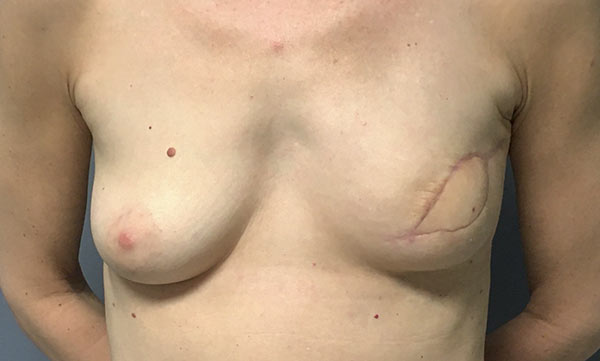
TUG Flap Breast Reconstruction
The TUG flap is an advanced technique in reconstructive breast surgery that uses tissue from a woman’s inner thigh to form a beautiful and natural appearing breast.
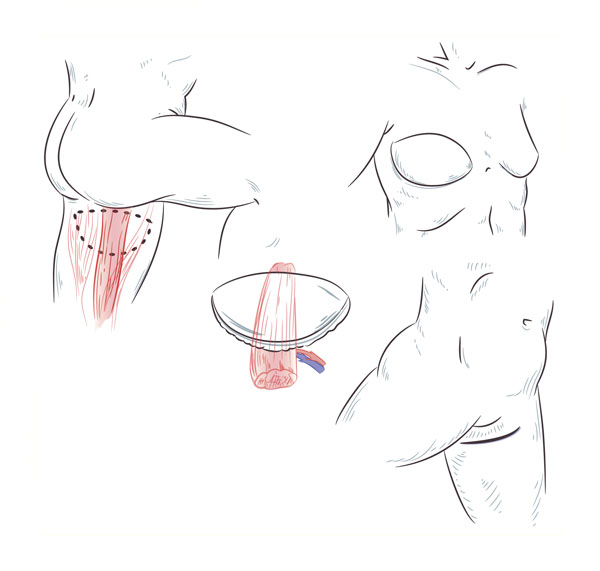
What is the TUG Flap Procedure?
Women who desire an autologous breast reconstruction but have insufficient abdominal tissue may be candidates for a transverse upper gracilis or TUG flap. A TUG flap uses a crescent-shaped area of skin, fat, and a portion of the gracilis muscle in the upper inner thigh to create a breast. The blood vessels supplying that tissue are identified and connected to vessels in the chest using delicate microvascular techniques. The thigh tissue is shaped to resemble a breast, giving a beautiful result with a natural appearance and feel. The thigh incision is well-concealed and can contour the thigh in the manner of a cosmetic thigh lift.

BENEFITS OF TUG FLAP BREAST RECONSTRUCTION:
- Natural appearance and feel
- Generally a better match to the other side, particularly if a woman does not want to alter the opposite breast.
- Ages more like a natural breast
- More reliable when the breast skin is damaged by radiation or surgery.
- Usually feasible even in thin patients with insufficient abdominal tissue to perform a DIEP
- Contours the thigh similar to a cosmetic thigh lift
WHO IS A CANDIDATE?
A woman who favors reconstruction with her own tissues may be a good candidate for a TUG flap. While the abdomen is the most common source of tissue in an autologous reconstruction, some women have insufficient abdominal tissue to undergo a DIEP flap. For those patients, the inner thigh is a good alternative if there is available skin and fat in that area. In most cases, the TUG flap is best suited to reconstruct a smaller breast.
In some cases, reconstructing the breast with living tissue is beneficial or even necessary. For instance, when the breast skin is damaged by radiation, recreating the breast from healthy living tissue can be more reliable and often produces a better result than an implant.
A TUG flap reconstruction requires a more extensive operation and a longer recovery, so patients should be in generally good health.
During your consultation, share your goals and priorities with Dr. Davison and Dr. Pinell. This will help them identify the best method of reconstruction for you.

TUG FLAP RECONSTRUCTION: WHAT TO EXPECT
- The first stage of reconstruction can usually be performed at the time of the mastectomy.
- If radiation treatments are planned, it is advantageous to place a temporary tissue expander at the initial operation. After radiation therapy is completed and the breast skin recovered, generally 6 months, a second operation is performed to remove the tissue expander and reconstruct the breast using a TUG flap.
- A one-sided TUG flap operation takes approximately 4 to 6 hours.
- Patients generally stay in the hospital for 3 to 5 days, but a complete recovery may take 4 to 6 weeks.
- Subsequent operations are often planned to refine the reconstructed breast, create a nipple, or to balance the opposite side.
Frequently Asked Questions
-
Can a TUG flap reconstruction be performed at the time of mastectomy?
- In many cases, yes. Immediate breast reconstruction is generally safe, produces the best aesthetic result, and is beneficial to coping with the loss of a breast.
- In some circumstances, it is beneficial to perform a TUG flap reconstruction at a later time, after a woman has completed all her breast cancer treatments. In these cases, a temporary tissue expander is often placed at the time of mastectomy to preserve the breast skin.
-
What are the risks of TUG flap breast reconstruction?
- Transferring tissue from the thighs to the chest requires the creation of new connections between their blood vessels. Even with meticulous microsurgical technique, there is an approximately 5% risk of clotting at those connections and flap failure.
- Other potential complications of a TUG flap include: bleeding (hematoma), infection, wound healing problems, and fat necrosis (hard knots that develop in areas of the reconstructed breast with poor circulation).
- Donor site (thigh) complications include delayed wound healing and fluid pockets (seromas). If only one side is harvested for a unilateral reconstruction, the contour of the thighs can be asymmetric. Because the gracilis muscle is one of five muscles that adduct the legs (bring them together), patients generally do not experience weakness of this movement following TUG flap surgery.
- Major blood clots (DVT, deep vein thrombosis or PE, pulmonary embolism) are uncommon but can be dangerous. To prevent this serious complication, patients are encouraged to get out of bed and walk soon after surgery, and are given blood thinners in the hospital and after discharge, usually for 2 weeks.
-
How long does a TUG flap operation take, and how long is a patient usually in the hospital?
A unilateral (one-sided) TUG flap reconstruction takes 4 to 6 hours. Patients are hospitalized for 3 to 5 days to monitor the flap and recover from surgery.
-
What is the recovery time following a TUG flap operation?
Patients should be out of bed the day after surgery and then gradually increase their activities from that point forward. While most women have resumed a modified daily routine by 2 to 3 weeks, a full recovery can take 4 to 6 weeks.
-
Are subsequent surgeries needed after a TUG flap?
Oftentimes, yes. Women will frequently undergo revision procedures to refine or enhance the appearance of the reconstructed breast. Nipple reconstruction and balancing operations on the opposite breast can be performed at that time as well.
-
Does a one-sided TUG flap create asymmetry between the thighs?
Some unevenness between the thighs can be expected if only one side is harvested. This is often addressed at a later operation with liposuction or skin tailoring on the opposite thigh.
-
Do the surgeons at DAVinci Plastic Surgery perform TUG flaps?
Yes! Dr. Davison and Dr. Pinell perform TUG flaps with technical expertise, artistic vision, and compassionate care. They have extensive experience with microvascular breast reconstruction and an outstanding record. In order to minimize patients’ time under anesthesia and to deliver the best possible result, these operations are always performed by both surgeons working as a team.
-
Does insurance cover TUG flap breast reconstruction?
Yes. All methods of breast reconstruction after a mastectomy and balancing procedures to the opposite breast are generally covered by insurance.